Our Office will be Closed Monday for Memorial Day
We'll re-open Tuesday, May 26 at 8am
JOHN K. - Baltimore, MD 21234
When it comes to hearing healthcare . . .
WHERE you decide to go
WHERE you decide to go
is probably the most important decision you'll make.
Our Doctors of Audiology use research-proven, evidence-based practices to help get the best possible results for our patients. We follow the science throughout the whole patient experience.
“I visited several other establishments before making a decision. The staff and facility at Harmony Hearing & Audiology is head and shoulders above the rest.”
Bob G. - Kingsville, MD - 21087
Diagnostic Testing - Hearing Aids - Adults - Pediatrics

Learn what Harmony Hearing can do for you
Meet our methods, people, and facility
Our Methods
The diagnosis and treatment of hearing loss is a science. As such, countless scientific articles have been published in peer-reviewed journals showing clinicians the best way to practice – if they want the best possible outcomes for their patients.
Unfortunately, many hearing clinicians ignore the scientific research.
If a cardiologist ignored the research, people would die, and they’d lose their license. But if a hearing clinician ignores the research, no one dies. People just walk around not hearing life as well as they possibly could – having no idea that things could be so much better.
If you want the best possible hearing healthcare, and we assume you do, you need to work with a facility and team that practices research-proven, evidence-based audiology.
We Use Real Ear Measurements
In-situ, probe mic, real ear measurements are used to determine frequency-specific amplification amounts when programming and adjusting hearing aids. Because everyone’s ear is shaped differently, the amount of sound that actually reaches the eardrum differs from person to person.
For example, considering two people with the exact same hearing aids and the exact same hearing loss, a 6’6″ man with large ears is probably going to require more amplification from a hearing aid compared to a 5’1″ woman with tiny ears. Although the hearing aid software displays how much sound is being pumped out of the hearing aid, what really matters is how much sound actually reaches the eardrum, and the only way to know that is to perform real ear measurements.
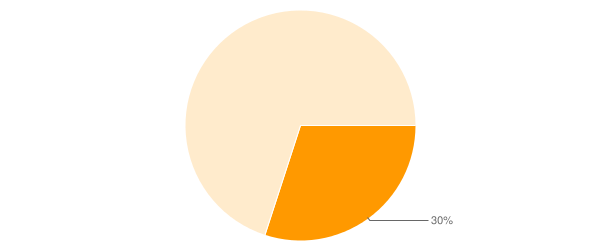
Only 30% of hearing clinicians routinely perform real ear measurements. (Mueller, 2014)
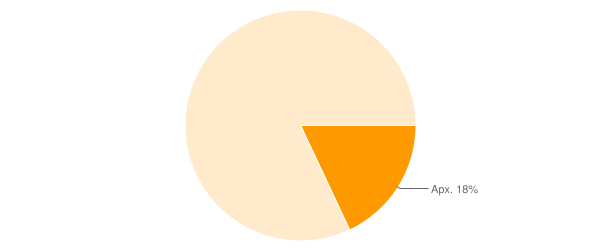
We Test Using Recorded Word Lists
Hearing is a lot more than how well you can hear a beeping sound. One part of the standard audiometric testing involves “word recognition”. The audiologist presents a list of words at a certain sound level, and the patient repeats the words back. This test can be used to assess hearing distortion, and unexpected changes in word recognition ability could indicate a more serious medical condition.
Researchers teach that word recognition testing should be performed using standardized recordings of word lists. This way, comparisons can be made across different appointments, offices, and clinicians. But most clinicians choose to present these word lists using their own voices through a microphone. Obviously, the test will be quite different, depending on who’s speaking, making accurate comparisons across different conditions impossible.
Only 18% of hearing clinicians routinely use recorded word lists. (Martin et al., 1999)

We Don't Rely on Default Hearing Aid Settings
When a hearing aid is initially programmed, they are adjusted according to the patient’s hearing test results by the manufacturer’s software. These default settings are known as the manufacturer’s “first fit”. But manufacturer “first fits” often emphasize comfort over clarity, and there is almost always room for improvement – if the clinician knows what kind of adjustments need to be made (using real ear measurements).
Many clinicians rely on the manufacturer’s default settings, but studies show that only about 12% of the time does the sound delivered to the eardrum match the prescription for the patient.
Hearing aid programming decisions need to be based on real ear measurement, patient feedback, and clinician experience – not manufacturer preferences.
Only 30% of hearing clinicians routinely alter initial manufacturer hearing aid settings. (Online survey reported by Beyer, 2011)
Our Clinicians
Molly B. Day, Au.D.
Doctor of Audiology
Hearing Clinician
Julia M. Yates, Au.D.
Doctor of Audiology
Hearing Clinician
Ally M. Ryan, Au.D.
Doctor of Audiology
Hearing Clinician
Matt Perry, Au.D.
Doctor of Audiology
Founder
Our Doctors of Audiology




“I would say that if someone was unhappy with the service they receive elsewhere, they should pay a visit to Harmony Hearing. After one visit, they won’t go back to their previous hearing center.”
Esther T. - Bel Air, MD - 21014
“I’ve been wearing hearing aids since the 1980’s, and I’ve been to countless hearing aid clinics. I have never had my hearing aids programmed as well as they did at Harmony Hearing. The equipment they used to program my hearing aids was unlike any I’ve ever seen. I came to them with hearing aids I had purchased earlier from another clinic. After they reprogrammed them, they are like a whole new pair of hearing aids. What a Difference!”
John K. - Baltimore, MD - 21234
Our Facility

We love technology. And when you visit our office, it’s obvious. It’s in the hearing aids we work with, the diagnostic equipment we use, and the multimedia equipment we use to review your test results and demonstrate hearing aids. We even have our own proprietary software systems that we’ve created to efficiently manage patient records and improve the patient experience.
Address:
Harmony Hearing & Audiology
Festival at Bel Air
5 Bel Air S Pkwy, Ste 1411
Bel Air, MD 21015
Contact Details:
Phone: (410)569-5999
Fax: (443)320-9468
Hours of Operation:
Monday – Friday
8:00am – 5:00pm